|
What If I Hadn’t Met You?
A Case Study of Working with Storytelling to Heal Birth Trauma Many families seek support during pregnancy, especially as they head toward labor and delivery. If a family has experienced birth trauma, defined as the feeling of or the witnessing possible threat to the life of the baby or mother during labor and delivery, they may seek the support of a therapist who specializes in trauma resolution (Simkin, 2016) . Studies have shown that for every woman who dies in labor, there are 70 women who almost die and many more that have painful, confusing moments that remain fixed in memory and in the body (NPR, 2018). I find that many women, their partners and their babies get overwhelmed during this time, and the way this can present clinically may be deceptive for providers. The science has shown that many women have their autonomic nervous system’s threat response come into play, which is more freeze than fight or flight, but can be both (Weinstein, 2016; APPPAH, 2019; Muzik & Rosenblum, 2017). Most often, there simply isn’t enough support to help birthing parents make sense of difficulty, provide a sense of presence and calm, and recognition of the different states that arise during birth for everyone: women, their partners, babies and staff. Working with the birth story that combines presence, pacing, and guided facilitation for parents and their children is a healing intervention. This case study employs the Healing Story, an intervention developed by Rebecca Thompson Hitt (Thompson, 2012; Thompson, 2019). The approach specifically focuses on integrating overwhelming birth experiences with a skillset combining presence, pacing, naming, and telling the story of the birth, what actually happened, and then how the parents wanted the birth to happen. Space is provided for the baby/child to participate in telling their version of the birth. Parents are coached to tell the story with their child, no matter what age. Children and babies often show their story, or participate with physical movement, play, sounds, emotions, and sometimes speech if they are old enough. The practitioner’s skills at facilitation include education about birth, birth trauma, the specific sequences of birth from the baby’s perspective, the importance of slowing the pace, somatic skills of presence, and reflective listening. I have combined Hitt’s approach into my many years of practice as prenatal and perinatal practitioner, especially the work of Ray Castellino, RPP, RCST®, creator of the Somatic Blueprint™ approach to healing perinatal trauma in families, and Mary Jackson, RN, LM, RCST®, SEP, midwife who also supports the using storytelling in working with families who have difficult births. This case study illuminates this process and provides a structure for healing birth trauma in families. The Family[1] Sharon came to do therapy with me at 25 weeks pregnant with her second baby because she had a difficult first birth and wanted a better experience this time. She also had a challenging life as a young adult due to the death of her mother when she was 13. This early overwhelming experience laid down a foundation of self-doubt that, when coupled with her difficult first birth, was troubling her and creating fear as she headed toward labor and delivery. She was a very healthy, fit young woman. During her initial intake she explained that “yoga had found her,” sharing that eventually she became a yoga instructor. I knew there was a place of trust and commitment inside her. Her husband, Steve, was a lovely man and very supportive of her healing intentions. My focus at this time was to settle Sharon, help her prepare for the birth of her second son. At the time of Sharon’s second birth, her first son, Nick was 2 years old. Perinatal Therapist Care Supporting parents during conception, pregnancy, birth and through early childhood is some of most important work we can offer for human development. Interventions include psycho-education, parenting, meditations, bodywork especially craniosacral therapy (all kinds), therapeutic touch and mindfulness. Hitt’s Healing Story approach includes the impact of birth trauma, and the parents’ and baby’s experiences of pregnancy and birth. Trauma during this time may impact the family so that relationships are ruptured. Without proper attention to and deep understanding of what happened, we can carry this sense of rupture and more into our lives where they become patterns of perceptions, beliefs and disease. I offer a healing approach that provides a sense of safety for the mother when she comes for her bodywork with me. Sharon came with fear and lack of trust from the birth trauma she experienced with Nick and from childhood trauma. While she wanted to also work with the impact of the loss of her mother on her life, I told her that the exploration of that loss can wait until she has had her baby. Stress management, support for decreasing the fear she felt and empowering her to trust her body were the focus of our sessions. Each time she came, I gave her prenatal massage, and crafted visualizations and felt sense experiences that supported her body and her baby. We differentiated from the first birth, recognizing how this experience is different and unique and supported that with sensation. Trauma held in the body is related to autonomic nervous system response to threat and is therefore very primal. So we spoke the language of the body (sensation), and with skilled facilitation trauma resolution, we transformed her fear into a more coherent state. Whenever fear came up, we gently processed it using a combination of presence, verbal skills, and touch. We communicated with her baby in utero (her second son), and prepared for her birth. At 38 weeks, the baby turned breech, which was a nightmare for Sharon. She felt she was repeating the pattern of her first birth where her first son also turned breech. An external version was successful, and she went on to have an optimal birth with him. One of her intentions was to hold her baby in her arms after birth, something she didn’t get a chance to do with Nick. Nick’s Birth Story Sharon shared with me her concerns of her first son, Nick. He often had night terrors and woke up crying, asking for her husband instead of her for comfort. She explained that Nick often wanted the support of her husband when he felt scared or hurt as well, and that bothered her. When she shared Nick’s birth story with me, how difficult it was and how he was in the NICU, I explained that many babies who have these experiences of separation from their mother at birth need a repair of that experience. I introduced the notion of the Healing Story at that time, or telling the story of the birth, then retelling the story, saying that she didn’t want him to be separated from her at all. I sent her instructions, and she completed a short version of this storytelling. She reported that Nick starting seeking her out for comfort more often, and that both she and her husband noticed. Sharon explained that she wanted a natural, vaginal birth with Nick. She, herself, had been born via c-section. The mother’s and father’s own birth experiences can influence the current time from an implicit, unspoken place. Sharon knew that C-section is not optimal. In her commitment to health, she knew intellectually that natural births were better for babies, and she wanted that for herself, husband and her baby. The couple enjoyed the preparation for Nick’s arrival, taking a 12 week birth preparation, which Steve later described as “incredibly romantic.” She chose to deliver in a hospital with a midwife. She described her labor as “legendary” in that hospital, as one nurse described it as the longest spontaneous labor in recent history (45 hours). Even though Sharon and Steven prepared well for birth, Nick turned breech at 39 weeks, which they were able to work with using an external version (doctor assisted turning of the baby head down.) Sharon described this procedure with great care, saying the staff took her condition quite seriously and supported her in feelings of concern. The version work and she went into labor spontaneously two days later. As she started having regular contractions, her doula came to the house. When her water broke after 8 hours of labor, there was meconium in the water. It was a slow release of water, with intermittent gushes. She labored a dozen hours in and out of the tub, with lots of movement. She reported that she vomited a lot (several times an hour for hours) so she needed fluids. They went to the hospital where she received an epidural after 20 hours of labor. She then slept 8 hours. Her labor continued until the afternoon the next day. At this point, after nearly two days of labor, she was checked and told she was at 4 cm, which was difficult news after all the time and hard work of the past 40 hours. They prepared for possible cesarean section at that time, but when she was checked again at 6 pm she was nearly fully dilated (“it was like magic,” Steve reported). The baby was reporting heart decelerations, and Sharon pushed for an hour. Nick was born just a few minutes before midnight, on the anniversary of her mother’s death. Sharon said she looked at the clock, and this moment impressed upon her because her mother died just a few minutes before midnight on the same day many years before. Nick had the cord wrapped around his neck. His weight was 8 lbs 13 oz and Apgar scores were low (4) and then went up to an 8/9. Sharon explained she was able to hold him for a minute before the pediatric team took him to the NICU. Her husband went with the baby. She had a 2.5 degree tear and had to be stitched. For any woman who has had this happen, it is a huge shock. Women often report feeling very alone in the birthing room without their mate or baby. From the baby’s perspective, the separation triggers a survival response. Depending on the condition of the baby, he will protest. His nervous system will report extreme threat, and his body will respond by shutting down. Nick was brought back to Sharon after 18 hours in the NICU after observation. From Steve: About the NICU experience Shortly before midnight, a feeling of seriousness came into the room. The Midwife was still in charge, but doctors had gathered around us. When Nick was born, he was handed to me; the Midwife asked me to announce if the baby was a boy or girl, then almost in the same second helped me place Nick in Sharon's arms. I was given scissors and urged to cut the umbilical cord. Sharon cried joyful tears as she held Nick, saying, "o my sweet baby, mama loves you so much." She was caught off guard when the doctors ended the moment so soon. They said they needed to take Nick because he was not breathing normally. It was something to do with his cry, which was not the right sound. The doctors put Nick on a cart, in a clear sided tray, with heat and lights shining on him. As they were preparing to leave the room they told me to come with them; I think I kissed Sharon and said I would be back and everything was going to be ok. We moved quickly down the hallway, to the elevator. I kept looking at Nick, and I think touched his foot or hand and told him I was his dad. The whole time I cried. Everything felt like it was moving by fast. Nick was always in focus, though. I had that dizzy feeling that comes when you cry a lot. We went into the NICU. It had a gray/blue dim vibe, almost like what you could imagine the inner of a space ship might look. Everyone in there was very kind and sweet. The doctor immediately put an oxygen tube into Nick's nose, an IV on his arm, and a monitor on his chest. Nick was hooked up to a machine that measured the strength of his breathing. They said it could be a while until he was strong enough to remove the oxygen tube from his nose and suggested that it might be a day or two. I think they ended up removing it after just a few hours because he was breathing well. I held Nick's hand a lot and kept looking at him, completely in awe. I could not believe how much I loved this baby right away. I spoke to him continuously and said that his mom and I loved him, and that his mom wished she could be there, and that she was getting better and we would all be together soon. I felt like I was both providing an incredibly supportive and necessary role to Nick right then, and knew there was no other option, but at the same time, I felt aware that I was the fortunate one to be with him. I was worried for how Sharon would feel; there was nothing more in the world she would want to be doing than to be next to him; holding him. I recorded a short video of Nick and left to show Sharon, and assure her everything was going to be ok. It was 1:30 am or 2:00 am, and Sharon watched the video and asked for every detail about Nick. Instead of tears of sadness from not being with Nick, she was full of amazement and joy. We celebrated that we had this amazing little boy with complete faith that he would be healthy soon. My the fear during the walk from the NICU back to Sharon's room of this being a big, painful event for our family, was eclipsed because I saw that Sharon knew Nick was going to be ok. I was relieved that she permitted herself to feel happiness first and foremost. It was all still a scary time, but it was not full of fear. It was immediately apparent that even though there was physical separation, a side of Sharon shone through in a way that I had never seen before. Still, to this day, I see in moments that same connection between Sharon and Nick. The next time we went back to the NICU, Sharon was with me. It was perhaps 2 - 3 hours after Nick was born. We visited him for 20 minutes, then fell asleep in a new hospital room. We woke up a few hours later, returned to the NICU and I think Sharon may have started breastfeeding Nick at that time. After a few more trips to visit him throughout the day, the doctors let Nick move into our room. It was around 3pm-5pm; Nick had been in the NICU approximately 15-18 hours. From Sharon: Reflection on Nick’s Birth It is really interesting to think back and consider what we were hoping for Nick’s birth. When I was pregnant, Steve and I took a 12 week Bradley method class together, which had been focused on aiming for a birth with the least amount of intervention possible. We learned extensively about prenatal development, practiced different types of breath work, and learned about a variety of natural comfort measures for labor. After that 12 week course, we were chock-full of knowledge so to speak. Intellectual knowledge and understanding, however, doesn’t always translate to deep emotional awareness or a felt sense about the experience that was coming. In some ways, when I think back, I feel as though I was actually afraid to even hope for a positive birth experience. I just felt like it was something that wasn’t possible for me. This is where that ingrained and narrow pattern of thinking kind of emerges. I didn’t really let myself dream about what Nick’s birth could be like, or what I wanted it to be. So his birth sort of became a test. Maybe almost to see what we were capable of handling. I certainly didn’t anticipate sitting in the tub for 10 hours and making no progress with my labor, or throwing up several times an hour for nearly 35 hours And requiring IV fluids, or an epidural to prevent maternal exhaustion. As my labor went on and on, the one thing I think I fixated on the most was trying to avoid a C-section, and that became my focus. It’s interesting to, that prior to Nick’s being born, I also didn’t envision what it would be like to hold my newborn baby on my chest, so perhaps it’s not a surprise that that didn’t happen either. I recall writing in Nick’s baby book that I almost didn’t believe in his existence until he was actually born. It makes me so sad to think back on that version of myself that was afraid to love something so much due to the fear that something could go wrong. Jason’s birth (her second son) certainly illuminated for me what can be possible with birth for both the mother and the baby, and has allowed me to reflect on my thoughts and feelings about Nick’s birth in a much deeper way. With regard to what I would’ve wanted for Nick’s birth, I guess I would say that most importantly, I wanted to hold him and to be able to try to feed him right after he was born. After such a long and exhausting labor for him and me, I feel like that connection and bonding would’ve been healing for both of us. I don’t necessarily find it helpful to think back about wishing that I had and needed so many interventions, etc., especially since after 45 hours of labor, and pushing for one hour, he was born several minutes before midnight on the anniversary of my mom‘s death. That, I think, has actually given me some peace about the whole experience. The fact that there was some kind of cosmic intervention that brought Nick into the world in the same space of time in which my mom left it. That is certainly helped me accept that whole experience. Using the Healing Story Steve and Sharon came in with Nick for a session to heal their birth experience. I had coached them on the phone the week before to think about how to tell the birth story simply and slowly to Nick with pauses, and then to tell the story again, the way they wanted it to go. Nick was rambunctious and curious. Like many small children who first enter my office, he went about exploring all my toys and looked into every nook and cranny. We finally settled down to tell the story. Steve and Sharon had obviously worked on what they wanted to say. I could tell it was hard for Sharon. As they told the story, I came in a few times to call pauses, slow the tempo, and have them reconnect through eye contact with each other and me. Sometimes, I would simply repeat what they said, directly connecting with Nick, with a statement like, “Yes, Nick, you and your parents had this experience, but that is not what they wanted for you.” Nick made himself busy climbing up and down on the couch, and in and out of their laps. Sometimes he started toward my shelves of toys, but he would often turn back and resume climbing in and out of his parents’ laps, going back and forth between the two of them as they sat on the couch. He often smiled and laughed. I could see that Sharon in particular was working really hard to connect with Nick, staying present with her feelings. In the Healing Story, we make space for feelings to come up and be felt. Like a wave, emotions in will rise and fall. We slow the pace, connect and make space, and the moment passes like an in and out breath. In the simplest way, Sharon and Nick explained what happened. When it came to telling Nick of how they wanted the birth to go, the room changed. The pace of Nick’s play slowed and he climbed into his mother’s lap and stayed there. As they finished telling him how they wanted it to go, and Sharon was able to say how she wanted to hold him after the birth and not have him be taken away, Nick began an interesting play pattern. He would point to different parts of his body –his knee, his elbow—and say, “boo boo.” And Sharon would kiss the boo boo. He also played a game where his mother would pretend to eat his finger, and they would laugh and laugh together. The father watched and smiled. Nick would smile, laugh, arch back, then stick his finger out to be eaten, and then point somewhere on his body and say, boo boo where upon his mother would offer him a kiss. Making Repair for Difficult Births The Boo Boo and Kiss game solicited by little Nick could be seen as a form of “repair” for a rupture in his birth sequence. A rupture is really a misattuned moment when the person in relationship does not feel seen, heard, felt, safe or protected. They can also get the sense they are unlovable or that they don’t belong. This birth was hard for everyone, parents, Nick and the birthing staff. In the Healing Story, the idea is to say to the baby/child, “This is how the birth went, it was not what we wanted. We are so sorry. What we wanted was to be with you, to hold you, to never let you go. We never wanted you to feel hurt, ever. We love you. We are so glad you are here.” When there is difficulty in birth and the baby feels hurt, confused, abandoned or scared the baby does not know how to make sense of it. Often, this can translate into not feeling wanted, or that is was their fault, or that they deserved the pain and suffering somehow. For those of us who study prenatal and perinatal somatic psychology, we know that these feelings can start prenatally or even in the previous generations. The baby responds with an array of emotions and actions associated on a continuum of threat responses. Babies can be angry, can push people away, arch, and communicate their feelings through body movements. Their bodies may become rigid or flaccid, cold or hot. Babies can become agitated, hard to soothe and settle. They can have difficulty feeding, connecting, and/or moving. Nothing a parent does feels right, so the parent then can go into a spin, feeling inadequate and helpless. These feelings can be coupled with their own pain and suffering from the birth experience. If unrecognized and not treated, the rupture can fester and grow, and often repeat in different ways as it seeks healing. The work I do is about recognizing patterns of rupture of relationship starting preconception through the first year of life. These experiences are profoundly somatic, as the left brain has not formed in the baby. Therefore memories are implicit and lie in our bodies. They form a foundation in the nervous system and may form a template for health lifelong. Somatic implicit memories can be easily ignited if current conditions are similar to those that originally happened. Birth patterns show up everywhere, especially how we make transitions, how we connect with ourselves and others, or how we handle stress. They show up in the messages we have for ourselves, our inner voices, our children, our mates, our society and culture. Once the patterns are recognized, we work to repair the difficulty and reconnect the family to each other and their whole experience of themselves. In essence, our work is about recognition, repair and connection. What If I hadn’t Met You? Sharon later told me that after the Healing Story, she started bathing Nick in the evenings and putting him to bed. Previously, Nick would only allow his father to do that. I encouraged Sharon to make special time for Nick. The birth of her second baby, Jason, has been a little challenging for him, his mother reports that Nick lets her soothe him. On a return visit, she said to me, “What if I hadn’t met you?” I smiled and knew that if they hadn’t learned the Healing Story, the pattern of rupture at birth would continue to seek healing. Social neuroscientist Mark Brady calls this the Integration Imperative; trauma seeks healing. Peter Levine, creator of Somatic Experiencing®, will say that trauma stored in the body will create a way to be heard, through pain or illness, emotion or gesture, it will speak in its unspoken voice. Perinatal trauma specialists are trained to see the pattern and hear that unspoken voice. Healing wants to happen, the pattern wants to be seen and the voice wants to be heard. If Sharon hadn’t met me, the story of the rupture would have stayed alive in the family, perhaps shifted or changed shape, but the theme of disconnection might have continued. With the prevalence of difficult births, trauma, and disconnection in our families, the Healing Story and other interventions that encourage repair, connection and integration of these painful experiences are key. The family can then move into feeling more whole and get off to a better start. Our family life is formative; children create the bodies and their minds in that space, and parents grow there, too. If you have had a difficult birth, seek out sensitive help, and you, too, can heal. References: APPPAH (Association for Prenatal and Perinatal Psychology and Health). (2019). Perinatal trauma-informed care practice panel, online seminar, retrieved from https://birth-psychology-classwomb.teachable.com/p/perinatal-trauma-informed-care-practice-panel Muzik, M. & Rosenblum, K. Eds. (2018). Motherhood in the face of trauma: Pathways towards healing and growth. Cham, Switzerland: Springer International Publishing. NPR. (2018) Lost Mothers: Maternal Mortality in the US. [Radio Broadcast]. Washington, DC. Simkin, P. (2016). Resource guide: Prevention and treatment of traumatic childbirth. Retrieved from: http://pattch.org/resource-guide/traumatic-births-and-ptsd-definition-and-statistics/ Thompson, Rebecca. (2012). Creating Connection: Essential Tools for Growing Families from Conception, Birth, and Beyond. (Book 2 of the Consciously Parenting series.) Crystal Beach, FL: The Consciously Parenting Project, LLC. Thompson Hitt, Rebecca. (2019). Healing story circles: How you can heal yourself and others through listening in community. Part of the Introduction to Prenatal and Perinatal Dynamics training. Retrieved from https://prenatal-and-perinatal-healing-online-learning.teachable.com Weinstein, A. (2016). Prenatal development and parents' lived experiences: How early events shape our psychophysiology and relationships (Norton Series on Interpersonal Neurobiology). NY: Norton Press [1] Names have been changed to protect confidentiality
0 Comments
April 2016
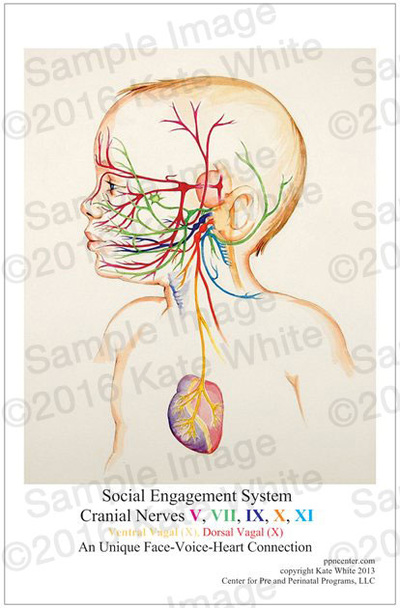
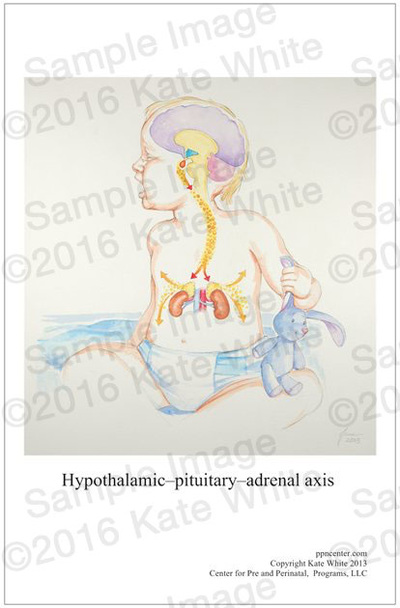
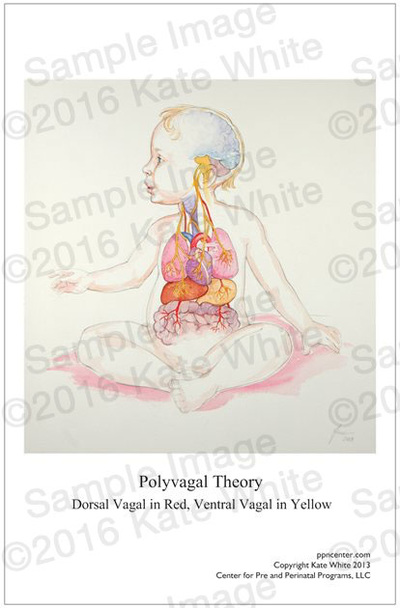
The Center for Prenatal and Perinatal Program announces that the Association for Prenatal and Perinatal Psychology and Health (APPPAH) is collaborating to promote its premier educational poster series on bonding, stress, social engagement and the polyvagal theory. These four posters feature beautiful images showing the intimate connection between mother and baby, and the neuroanatomy and physiology of this bond so that pediatric and maternity professionals can have attractive visual tools. The Director of the Center, Kate White, created the posters last year as part of her educational platform for professionals. She has been working with APPPAH for 3 years now. They approached her about working with the Center's products to support their new Somatics educational online program. Under the direction of Ms. White, APPPAH is offering an online education program, the Prenatal and Perinatal Educator Program that includes 11 competencies in early health: Foundations, Ethics, Epigenetics, Neuroscience, Pyschological Theories, Culture, Learning and Bonding, Labor and Delivery, Supported Attachment and Breastfeeding, Parenting Styles, and Implications and Inspiration. In 2014, White brought together over 30 advanced interdisciplinary professionals who have all been trained to work with early trauma starting preconception, during the prenatal period, birth, and attachment. These professionals each are qualified to teach APPPAH's new blended learning class on Somatics. Participants can learn ways to presence the physical elements that accompany relaying information about the early period. Because the early period has implicit information, or experiences that are encoded in the body and are often not made sense of by explicit or declarative memory, teaching about this early model of trauma and healing can be tricky. Educators are trained in how to deliver material, as well as what it is. The posters will be accompanied by a User's Guide so that professionals can easily learn the most important points about each subject, including practical applications, and a locked powerpoint so that each educator will have an electronic visual for seminars and workshops. For more information see http://www.birthpsychology.com. Have Babies Will Travel: Award Winning Educator Launches New “Sensational Baby” Program
At first you do a double take; are those real babies in that bag? But then the carrier notices your look, and smiles. “They’re dolls,” says Certified Infant Massage Instructor Kate White, “But I know they look real.” White is the Director of the Center for Prenatal and Perinatal Programs, a center in downtown Charlottesville,VA committed to increasing prenatal and perinatal outcomes through education, therapy, research and communication. She is currently offering a new educational program for mothers, fathers, caregivers and precrawling babies. The “Sensational Baby” program was recently launched by Infant Massage USA, the US chapter of the International Association of Infant Massage (IAIM) in Sweden that certifies professionals in baby massage. It has over 10,000 members worldwide. Originally started by Vimala McClure, the International Association of Infant Massage’s mission is to “promote nurturing touch through training, education, and research so that babies, parents, and caregivers are loved, valued, and respected throughout the world community.” The USA chapter was started in 2005. The IAIM is the largest infant massage organization in the world, with international conferences and trainings in many countries. “I started working with mothers and their babies in 1995,” explains White, who had a career in Africa working to improve maternal and child health before becoming a massage therapist. She returned to the United States in 1992 and entered massage school so she could have a physical skill to help pregnant women. “I wanted to help women in my own country,” she explains, after spending many years working to improve clinical and national conditions for maternity care in other countries. “Prenatal and infant massage were the first two things I studied right after completing my basic training in 1995. I have been working with pregnant and postpartum mothers, and families with newborns ever since.” The Center is White’s second educational space dedicated to helping families with babies. She ran a healing arts center dedicated to the pre and perinatal arts in Vermont for many years before moving to central Virginia. She worked with a midwife there preparing couples for childbirth and then helping them with their babies afterwards. Her classes include information on attachment, bonding and the neuroscience of connection, along with finger plays, lullabies, and information on the developing nervous system of babies. She also offers TummyTime!™ classes that help improve babies’ experiences of being on the stomach, a position that is often uncomfortable for babies but recommended for improved development. She has spent many years now studying pre and perinatal education, and also serves as Director of Education for the Association for Prenatal and Perinatal Psychology and Health. This organization recently honored her with the Outstanding Educator Award for her contributions in creating, managing and teaching an international program that has over 180 students in 25 countries around the world. Other organizations have recognized White for her contributions to improving the culture of birth in central Virginia. She has worked locally in the Charlottesville area since 2008, when she began a local collaborative of perinatal professionals. Representing Birth Matters, VA a statewide nonprofit that seeks to improve the culture of birth through birth circles, educational offerings and speakers, White organized large health fairs to educate couples about birth options and local services, receiving the 2012 Advocate of Year award for her efforts. “Recently, a client asked me what my favorite thing about my work is,” says White, “I answered, taking care of pregnant women and their babies.” Her private bodywork practice, Belvedere Integrated Healing Arts, has a special program for pregnant and postpartum mothers she calls MotherCare, “because when you support a mother, you care for the world,” the brochure states. And White is very clear about that. “Mothers make the next generation,” she says, “It is one of the most important jobs on the planet. And if we support them, then we can support their babies and the support can continue into the next generation.” For the baby massage, Sensational Baby is a 4 or 5 class series for families with precrawling babies. There are many benefits, including promotion of bonding and attachment, improving sleep, better digestion, decrease in pain, and increase of immunity. “There are so many benefits for the baby,” says White, “and for the caregiver. It is a time when mothers’ brains can change as they go into deep relationship with their baby. I spend a lot of time teaching about how babies communicate. It is primarily nonverbal. I help parents learn about their baby’s experience, how to communicate their caring through touch, relieve gas pains, and facilitate healing of anything difficult that might have happened prenatally or during birth. Loving touch is a great way to help create peaceful human beings.” One of the hallmarks of this curriculum is teaching how to ask permission of your baby to complete massages, acknowledging that babies have preference in relationship with their caregivers. White’s expertise includes bodywork to help with breastfeeding. “Breastfeeding is a full body experience for a baby,” she explains, “Many times, breastfeeding can feel uncomfortable for mom and baby. Bodywork can help sort that out.” Her training includes many years of craniosacral therapy, a very light form of bodywork that helps decompress key areas of a baby’s body to improve nervous system function. “Key nerves can get compressed that play a role in nervous system regulation. The bodywork I offer helps with reflux, gas, pain in the neck and shoulders, as well as hips. It is more than any one therapy,” White explains. “It is a mixture of manual therapy, pacing, tempo and communication with the baby. Parents learn a lot in the sessions with me. And I love helping them.” So if you see a woman walking around Charlottesville with a bag that looks like it is filled with babies, don’t be alarmed. It is just White off to teach another class or do home visit to help a family learn more about their baby. More information about infant massage can be found on the IAIM website, http://www.infantmassageusa.org/. |
AuthorKate White, MA, CMT, RCST, SEP is a massage and craniosacral therapist in Charlottesville, VA. Archives
September 2019
Categories |





 RSS Feed
RSS Feed